
With the changes in etiology, MPP shows new epidemiological characteristics, manifested as specific imaging changes that affect the pulmonary ventilation function (PVF), but the obvious pathogenesis is still unclear. 
MPP has been well recognized as one of the most critical and dangerous health problems all over the China. 
However, reports vary by age, region, year, and year of prevalence, so there are various reports with similar results. At present, the diagnosis of MPP in China mainly relies on serological tests. For a definitive diagnosis, testing for the pathogen is required. The clinical manifestations and chest X-ray examination of MPP are not characteristic, and the diagnosis cannot be made based on the clinical manifestations and chest X-ray examination alone. Data show that MP infection accounts for 10–40% of community-acquired pneumonia (CAP) in children at 9–14 years old, with a peak age of 4–6 years. The incidence rate of MP infection has shown an upward trend year by year, which has been proved by related studies in recent years. The diseases are mostly spread by respiratory droplets, and sporadic infections occur throughout the year, especially in late autumn and early winter. Mycoplasma pneumoniae (MP) is well-known as an intracellular pathogen that can cause respiratory diseases and extra-pulmonary diseases of children, which is commonly named as mycoplasma pneumoniae pneumonia (MPP). Pulmonary HRCT and PVF can be undertaken as important indicators to judge the severity and prognosis of MPP in school-age children. In children with MPP, both the large and small airways were affected, but the recovery of the small airways was slow. Compared with the case in acute phase, the PVF indicators of children in the re-examination phases were much higher, with greatly statistical differences ( P < 0.05). Compared with the group with normal HRCT results, the forced vital capacity (FVC), forced expiratory volume in 1 second (FEV1), peak expiratory flow (PEF), forced expiratory flow at 25% forced expiratory volume (FEF25), forced expiratory flow at 50% forced expiratory volume (FEF50), forced expiratory flow at 75% forced expiratory volume (FEF75), and maximum mid-expiratory flow (MMEF75/25) of children in bronchopneumonia group, segmental pneumonia group, and lobar pneumonia group were obviously reduced, showing statistically great differences ( P < 0.05). In addition to the above symptoms, children with MPP had different degrees of PVF impairment. 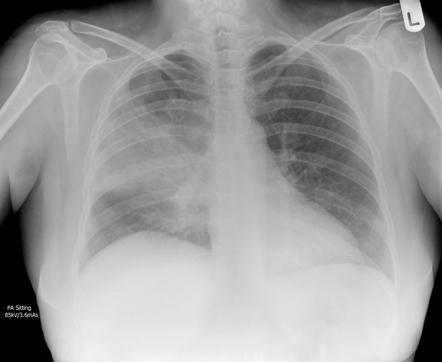
Clinically, the children with MPP suffered from fever, cough, and sore throat. Relevant indicators were statistically analyzed to determine the change rules of chest HRCT and PVF and correlation between the two. The chest HRCT and pulmonary ventilation function (PVF) were examined in the acute phase, the second phase re-examination period, and the third phase re-examination period. 71 children hospitalized with MPP were undertaken as the research objects to observe the incidence rate, occurrence time, and duration of the clinical symptoms and pathological signs. This study was aimed to explore the diagnosis and prognosis of mycoplasma pneumoniae pneumonia (MPP) in children using high-resolution computed tomography (CT) (HRCT). Pneumonia symptoms in at-risk patients, such as older people and those with dysphagia or impaired neurologic status (e.g.Mycoplasma pneumoniae (MP) is defined as a common cause of pulmonary infections and accounts for up to four over ten of pneumonia in children over age 5.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
